|
Development of a referral system using kangaroo mother care for low birth weight babies
PI: Hadi Pratomo, Faculty of Public Health, Universitas Indonesia
USG-Supported Partner: Abdullah Baqui, Johns Hopkins University Bloomberg School of Public Health
Project dates: February 2015 - December 2018
Project Overview:
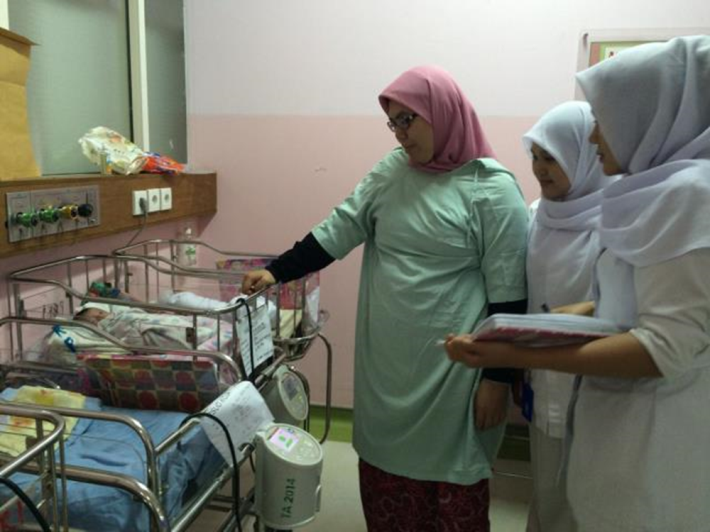 | Observation in Perinatology Unit at Koja Hospital. (photo courtesy of PI Hadi Pratomo)
|  | Home visit to low-birth weight infants (LBWI) post hospital care at Koja Hospital - Kangaroo Mother Care (KMC) is not continued at home. (photo courtesy of PI Hadi Pratomo)
|
The project aims to improve the survival of low birth weight infants (LBWI) using kangaroo mother care (KMC). The objectives are to address LBWI problems, improve the referral system from community to hospitals and vice versa, promote the sustainability of the KMC for increasing its survival, as well as reduction of both mortality and morbidity. The referral health system has been developed by the Ministry of Health. However, the implementation of this services including LBWI is still a big challenge. Coordination and follow-up of referral services after discharge from hospital is very weak. Through current policy on Universal Coverage of health services (BPJS), there is an opportunity to devise and strengthen the referral health system including cases of LBWI. The design of the study is a before and after intervention and is carried out at the hospital and community levels. The primary target population is families with LBWI born in either the hospital or community setting. In each district, the expected number of mothers with LBWI is estimated at 200 in each hospital, 100 in either primary health centers or private midwife clinics, and another 100 born at home delivery. The total sample will be approximately 800 mothers with LBWI. The secondary target populations are family members, cadres, health care providers, and decision makers. The formative research will be conducted to increase the possibility of an effective, acceptable, and sustainable intervention. Also, it will fine tune the proposed intervention adjusted to the existing condition. A quantitative study will follow with the aim to investigate LBWI survival and morbidity rates. Case fatality rates (CFR) due to major complications and neonatal mortality will be studied retrospectively both at the hospital and community settings. However, both neonatal morbidity and CFR will only be studied at the hospital level. The intervention will consists of Learning Organization, and training for personnel who will be involved in the care of LBWI for KMC and its referral system. An end-line study will be conducted to compare the knowledge and perception about KMC services and referral for LBWI using KMC before and after the intervention.
The primary outcome measure is improvements in LBWI outcomes such as survival, presence of complications, CFR, and cause of death after graduated from or receiving some KMC service. The secondary outcome measures include improvements in knowledge, opinion, and perception of health personnel about KMC and LBWI referral using KMC. To monitor implementation, several tools will be developed such as KMC admission criteria both in hospital and in the community setting.
The USG-Supported partner has extensive experience in the interventions to improve perinatal and neonatal survival in developing countries. Therefore, through this collaboration the research team will gain experience in conducting quality research in newborn care and publishing in the international journals.
Final Summary of Project Activities
The project ended as of December 2018. The major project achievement was policy change regarding Kangaroo Mother Care implementation in Koja Hospital. Koja Hospital is determined to become a center of excellence for KMC in Jakarta area; therefore, they have changed their Medium Plan Strategies to highlight the KMC practice. They also established a room designated for KMC for mothers and equipment needed to practice continued KMC in the hospital. In addition, the information technology system using a web-based application, si Kanguru (Kanguru means Kangaroo), was also established to ensure information on LBW babies and KMC practices are available for monitoring purposes in the Koja area. Si Kanguru contains information on LBW babies collected during follow up visits done by community health personnel and can be accessed by both hospital and community health personnel to ensure the continuous care and KMC practice for the LBW babies. While Karawang is still considering policy changes regarding the KMC practice, it has showed their willingness to practice KMC in the hospital and uses the referral mechanism for monitoring and follow up LBW babies.
In order to achieve the research objectives, the team conducted a baseline assessment through Knowledge, Attitude, and Practice (KAP) surveys of health personnel which showed that they lacked in knowledge on KMC practices. A pilot training of KMC using the updated modules (from previous KMC modules in Malawi and Nepal) was performed in a hospital in East Jakarta prior to implementation in the study sites of Karawang and Koja Hospitals. Modules for community health personnel training were also developed. Training for health personnel in both hospitals covered 210 participants consisting of doctors, nurses, and midwives, as well as 247 participants from primary health centers (PHC) in both areas. Post training activities, implementation of KMC practice in both areas began which aimed to increase KMC practices in the hospital and the community.
Data collection on newborn mortality and morbidity of low birth weight babies in both hospitals occurred using registers from wards and medical records. This activity was followed up with home visits to the LBW babies’ houses and measured their growth and weight gain. Additionally, the team emphasized and supported North Jakarta and Karawang to set a referral mechanism from hospital to community for LBW babies discharged from the hospitals using KMC as means of transport and accompanied by community midwives during transfer from hospital to community. At the community, midwives also ensured that KMC was practiced by the family and monitored the babies’ growth and weight gain. The referral mechanism is now used by both areas and uses group messaging to share information on discharged babies and follow up plans. Through the monitoring and evaluation activity, the research team found that both hospitals have standard operating procedures (SOP) for KMC implementation, but not for KMC counselling. In response, the team conducted a panel meeting which included experts on KMC and pediatricians, as well as management teams of both hospitals to develop the SOPs. As a result, both hospitals have SOPs for KMC counselling.
For outreach, the team produced KMC media in the form of flipcharts and booklets. The flipchart and booklet have been distributed to Koja and Karawang hospital, and to all PHC in North Jakarta and Karawang districts. The booklet and flipchart have received intellectual property rights from Indonesia as of November 2017. A national level dissemination meeting was also organized in Jakarta with aim to disseminate the research results and findings and to obtain commitment from invited stakeholders to implement KMC for LBW babies. Meeting participants were from the Ministry of Health, Jakarta and West Java PHO, DHOs (North Jakarta, East Jakarta, Karawang), Province Hospitals in Jakarta, Perina Medica, and other stakeholders. A focus on improvements of LBW baby care through KMC was agreed to be implemented and scaled up. The Director of Family Health actively participated in the meeting and expressed her willingness to support the KMC implementation in Indonesia.
PEER Health Cycle 2 Recipients
|





